What makes telehealth work?

He oversees care coordination telehealth through most of the Rocky Mountains for the Veterans Administration, and he has learned the ingredients of success well. (Picture from Global Media.)
While the rest of the medical community flounders about trying to figure this out, here is what he says you need to make it work:
- A robust Electronic Health Record.
- A network that can handle the necessary bandwidth.
- Digital video systems that are simple to use but support a range of peripherals.
- A system integrator who can put it all together.
- Clinical staff in remote locations who know tech but are even better with people.
The VA is fortunate in that its VistA EHR has been around for decades. But that only gets you part of the way there. "We also have a closed network, we have a firewall, we have broadband to all our clinic end points. We have the luxury of solid bandwidth and the ability to do video over IP."
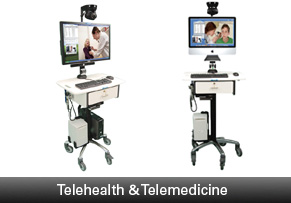
Beyond these institutional advantages, Lowe has standardized on Tandberg (now Cisco) codecs and cameras from Global Media of Scottsdale, Arizona.
"They have a cart system that can incorporate the codec, monitors, a computer, and all the peripherals, and they have a great cable management system that helps in small clinical spaces."
All these systems are maintained through a system integrator who can do installation and maintenance throughout the region.
"It's the integration of all these pieces that's the difficult part. A lot of companies make carts and cool innovations, but trying to assemble them into something that works for a clinician, at very remote locations with untrained clinical staff...it needs to be highly usable and highly reliable."
Several elements must be supported. The camera must have a wide variety of remote controls and you want to support a variety of peripherals like a digital stethoscope, an otoscope, even an ophthalmoscope, for taking remote measurements.
Finally, you need clinical staff in the remote office. Lowe says that at the VA this is a GS-7 rated, health tech, usually with a community college background. The ability to deal with the technology is important, but Lowe has also found people skills vital. "They are the hands and senses of the remote provider."
Once the system is in place doctors can do many kinds of evaluations from a very long way away.
"We do a lot of tele-mental health. We do a lot of patient education, which is a huge part of health care, educating on diabetes, smoking cessation, and nutrition. We do pre-surgical evaluations, and post-surgery follow ups. We do tele-endocrinology, wheelchair and prosthetic evaluations, even speech therapy."
Lowe and the VA have built this system out of need. With so many patients so far from a VA center, they can either do telehealth or let clients slip through the cracks.
But what he has found is that, with proper equipment and properly trained staff, he has a productivity gold mine. Doctors can provide a lot of services, efficiently, including wellness calls they might not otherwise be able to make.
And that's what drives down health care costs. It's not the equipment, but the human connection that counts. A remote clinical check-up has trained people on both ends of the line, and more people in support.