Study finds that robots are just as effective as human surgeons

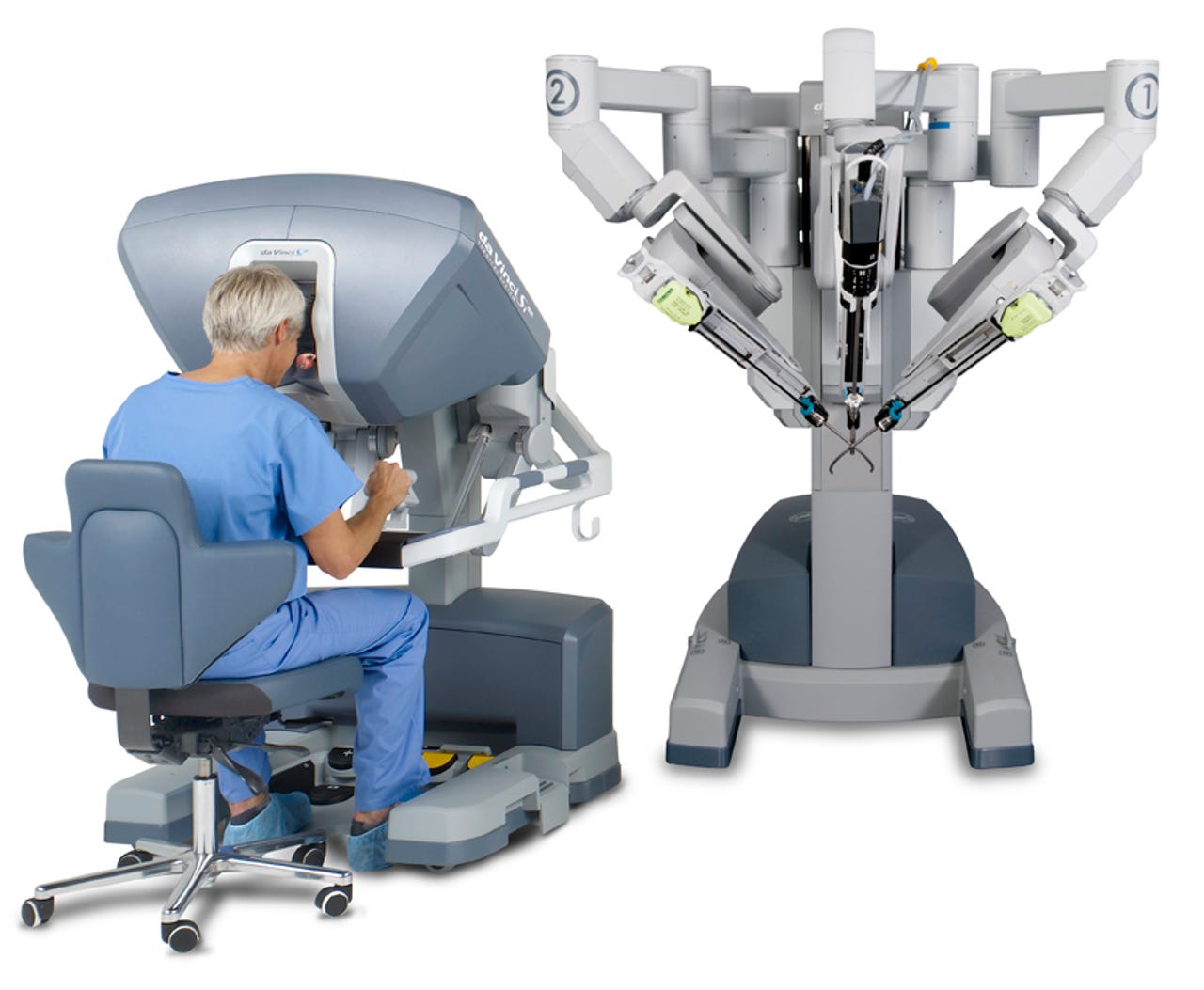
Image: Intuitive Surgical
Robotic surgery has skyrocketed ever since the Food and Drug Administration approved the da Vinci surgical system 16 years ago. Now, a study has proven that robotic arms and human hands are equally effective.
Surgeons commonly use the robotic system as a tool to help them perform operations. It is mostly used to treat patients who have been diagnosed with prostate cancer, which affects one in seven American men, according to the Prostate Cancer Foundation. Even though the robot comes with a $2m price tag, it is used to perform 80 percent of radical prostatectomies (operations to remove the prostate gland) in the US.
Read this
Compared to open surgery done with human hands, the procedure, called robot-assisted laparoscopic prostatectomy (RALP), is preferred by many surgeons and patients because it requires smaller incisions, which presumably translates to easier recovery. Traditionally, to remove a prostate, a surgeon would make a cut from the belly button down to the pubic bone.
With RALP, a surgeon sits at a control panel and uses robotic arms to perform the operation. The robot has a high-magnification 3D camera that the surgeon uses to see inside a patient's abdomen, while robotic arms make several small incisions. (Read: How robots are redefining the future of surgery.) Assumptions about whether robotic surgery is more or less effective than open surgery hadn't been verified until recently.
A study published this week in the medical journal The Lancet concludes that both robots and human surgeons achieved similar results. "Surgery has long been the dominant approach for the treatment of localized prostate cancer, with many clinicians now recommending the robotic method to patients," said lead author Robert 'Frank' Gardiner, University of Queensland Centre for Clinical Research, in a statement. "Many clinicians claim the benefits of robotic technology lead to improved quality of life and oncological outcomes." In reality, it seems that final outcomes are the same, whether a human or a robot performs the surgery.
The trial led by surgeons at the Royal Brisbane and Women's Hospital randomly assigned 308 men with localized prostate cancer to have either robotic surgery or open surgery. After assessing the patients three months post-operation, the researchers concluded that robotic surgery was just as effective as the human version.
On the upside, RALP patients experienced faster recovery times. They lost less blood during surgery, stayed in the hospital for a shorter amount of time, and reported better physical quality of life six weeks after the operation. Twelve weeks after the surgery, both groups of patients experienced similar results, as measured by urinary and sexual function, which are considered key indicators of a prostatectomy's success.
The long-term outcomes -- especially cancer survival rates -- have yet to be determined, and the study (funded by the Cancer Council Queensland) will continue to follow the patients for a total of two years.