Training computers to help detect pain

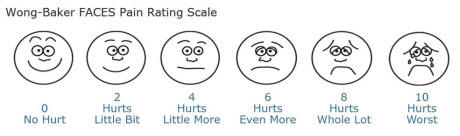
Image courtesy of http://www.wongbakerfaces.org
A research article published yesterday in PLoS ONE revealed promising work done by a Stanford University research team who has been using software to help parse information generated by brain scans, enabling them to detect when people are in pain.
Pain is one of the key elements of the patient assessment we nurses do. Assessing pain is so important, because pain is considered to be the fifth vital sign.
Pain is defined by the International Association for the Study of Pain as "an unpleasant sensory and emotional experience arising from actual or potential tissue damage or described in terms of such damage."
The way we nurses normally assess for pain is to teach the pain scale, which is to say we describe feeling no pain at all as a "0" and the very worst pain imaginable as a "10," and ask a patient to rate how they are feeling as a number on that scale.
We also try to get some details on the pain, such as what kind of pain it is (i.e., stabbing, dull, achy, etc.), when it started, what brings it on, where it is located in the body (for example, chest pain needs to be urgently addressed), and if anything seems to help it.
This pain scale system works very well if a patient is aware and cognitively able to describe what's going on. It's a bit harder with very young or old patients, patients with cognitive limitations such as dementia, or patients who aren't verbal for whatever reason.
We show little kids a cute chart with five faces on it, and ask the kids to point to the face which tells how they feel. We stay on the lookout for non-verbal indicators of pain, such as clutching and guarding areas of the body, grimacing, labored breathing, increased heart rate, etc. Unfortunately, sometimes patients who can't say they're hurting don't get helped.
We are told as practitioners of healing arts that the patient is to be considered as the authority on their own pain. We are cautioned to remember that people can experience pain differently. It has been said that it may even be true that no two people experience it exactly the same way.
Even the same person doesn't experience it the same way at different times. People with chronic, long term pain present differently than people with sudden onset, acute pain. Long term pain can manifest itself in depression. On the flip side, depression can manifest itself as physical pain.
One of the things that has made me angry in clinical environments is when I perceive patients being labeled by their caregivers as drug seeking because of their reports of pain, and then having their complaints dismissed. I try not to project this just because it's a pet peeve of mine, but I have seen it happen many a time.
I'm glad to hear that this California research team feels hopeful that the technology can eventually be used for better detection and treatment of chronic pain (although that level of granularity is not available at this point), as well as to help those patients who can't verbally express pain. In my opinion, it would be a great help to have an objective measure of pain to add to the mix of things we use to provide better care to our patients. I am encouraged by 84% accuracy, but am concerned about the other 16%.
Pain is an extremely important topic, since pain is one of the the main things that drives people to seek care medical care in the first place, and can amount to a major impediment to people's ability to move past illness into health.
If you're interested, read the details of the research, as well as the research team's recommendations on how to advance this physiology-based pain detection approach toward use in clinical settings.
What do you think of the idea of a computer helping to detect or corroborate reports of pain in patients? Please share in the TalkBacks below.